Top stories in Nova Scotia
Local
MoreOpinion
MoreBusiness
MoreLifestyles
MoreTwo Cape Breton music industry greats to be honoured at 2024 ECMAs
The East Coast Music Association (ECMA) is set to honour two well-known Cape Breton music industry members, Bruce Guthro and Stephen Muise, next month at the annual awards ceremony in Charlottetown, P.E.I.
Bruce Guthro, who passed away last ...
Updated 27 minutes ago
|3 min read
Sports
MoreCommunities
MoreCanada
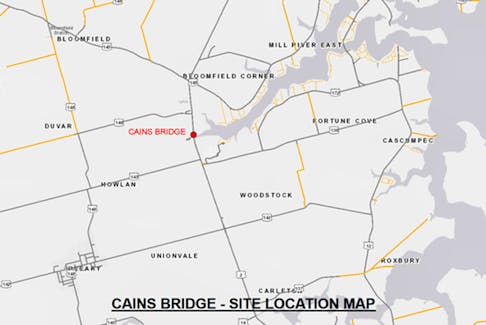
MoreTwo bridges in rural P.E.I. closing for construction
P.E.I. drivers in both Prince and Kings counties are being advised of two bridge replacements impacting traffic throughout the spring and summer.
Both Cains Bridge on Route 2 near Bloomfield Provincial Park, and Bridgetown Bridge on Seven Mile Road ...
Updated 50 minutes ago
|2 min read
World
MoreRFK Jr running mate injects needed cash in independent's campaign
By Stephanie Kelly (Reuters) - The role Robert F. Kennedy Jr.'s running mate, Nicole Shanahan, will play in his White House bid is coming into focus, as the wealthy lawyer injects millions of dollars into their independent campaign and amplifies ...
Updated 10 minutes ago
|3 min read